A dog skin infection caused by bacteria and a novel fungal pathogen, Trichocladium sp.
Narayan Paul, DVM, MS, PhD, Amy Swinford, DVM, MS, DACVM, and Julie Piccione, DVM, MS, DACVP
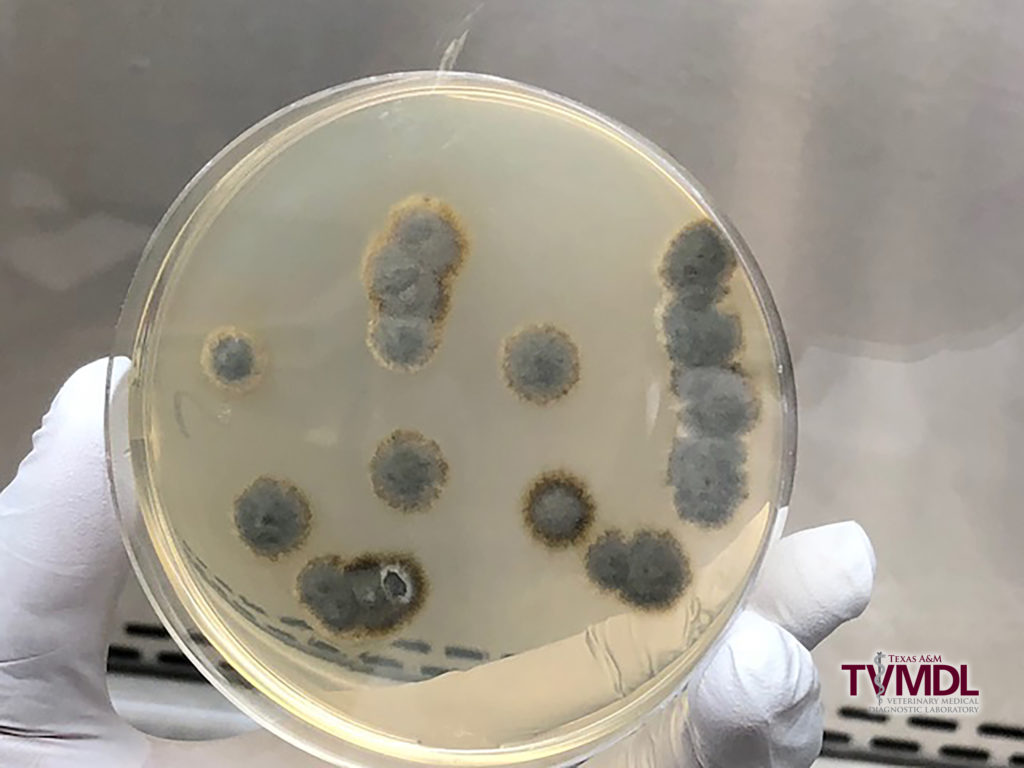
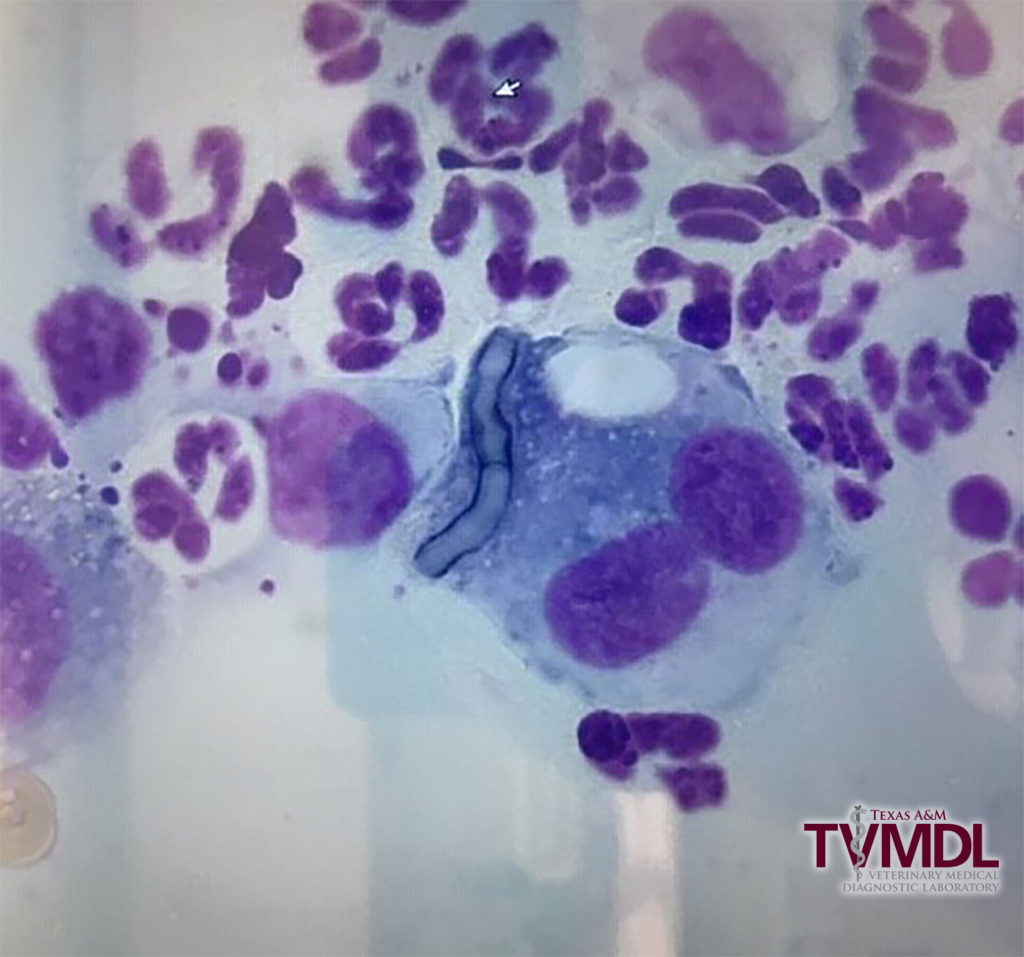
A nine-year-old female, spayed dog was presented to a veterinarian for diagnosis and treatment of a skin infection. The dog was treated with antibiotic and immunosuppressive drugs to resolve the infection. A punch biopsy sample was submitted to the Texas A&M Veterinary Medical Diagnostic Laboratory (TVMDL) in College Station for bacterial and fungal culture. Bacterial cultures revealed the presence of Staphylococcus pseudintermedius and Streptococcus equisimilis in the sample. Antibiotic susceptibility testing was performed on Staphylococcus pseudintermedius and identified this bacterium as a methicillin-resistant Staphylococcus pseudintermedius (MRSP). Fungal cultures produced a pure culture of a fungal saprophyte on several of the fungal media (Figure 1). A lactophenol/aniline blue stained slide mount of the fungus was examined microscopically in an attempt to identify the fungal pathogen morphologically. As the isolate was not able to be definitively identified by colony and microscopic morphology, DNA sequencing was performed to identify the fungus up to genus/species level by amplifying the internal transcriber spacer (ITS) region. Based on the findings, the fungus was identified as a member of the genus Trichocladium. In follow up communication, the client informed TVMDL that several fungal hyphae were observed within macrophages and amongst other inflammatory cells in cytology samples, suggesting clinical significance of the fungal isolate (Figure 2).
Canine skin infections can be caused by a variety of pathogens. MRSP is a major pathogen of dogs and commonly associated with a variety of skin and wound infections. MRSP is commonly found to be resistant to many antibiotics, and therefore treatment with appropriate antibiotics is very critical. In this case, the infection was complicated by the presence of a fungal saprophyte, Trichocladium sp. A search of the literature shows that this is primarily a plant pathogen and there do not appear to be reports of infections in humans or animals. However, as this fungus is common in the environment, one could speculate that the cutaneous infection was initially caused by traumatic implantation of plant material containing Trichocladium sp. into the skin, followed by a secondary bacterial infection.
To learn more about this case, contact Dr. Amy Swinford, Associate Director or Dr. Narayan Paul, Bacteriology Section Head at the College Station laboratory. For more information about TVMDL’s test offerings, visit tvmdl.tamu.edu or call 1.888.646.5623.